The dysregulation of nutrient-sensing mechanisms is a hallmark of aging. In vivo studies done on rats and other animal models show that calorie restriction can increase longevity. Rats that were subjected to calorie restriction also had a longer healthspan. (Whether this applies to humans has never been proven, but many longevity researchers suspect it does.) Four biochemical pathways are of interest: IGF-1 and the IIS pathway, mTOR pathway, sirtuins, and AMPK. Functionings of the pathways are influenced by nutrient levels. The four pathways influence aging as well as metabolism.
The insulin growth factor 1 (IGF-1 also called somatomedin C) has an affinity for glucose and it plays a role in the body’s glucose sensing. In vivo studies in mice have shown that inhibition of the IGF-1 pathway increases lifespan. Additional studies in worms and fruit flies have shown that a transcription factor FOXO (forkhead box protein O1) extends lifespan by suppressing the activity of the Insulin/IGF-1 Signaling (IIS) pathway. Studies on people with Laron syndrome (growth hormone deficiency) show that their naturally lower levels of IGF-1 activity enhance longevity. Experiments on yeast (S. cerevisiae species) show that an increase in IGF-1 and growth hormone signaling may promote oxidative stress and suppress apoptosis, leading scientists to suspect this mechanism could promote malignant tumorigenesis in multi-cellular animals. Oxidative stress increases DNA damage; accumulation of DNA damage leads to cellular senescence, untimely aging, and the development of age-related ailments.
The mechanistic target of the rapamycin (mTor) pathway is another nutrient-sensing pathway that is associated with aging. mTor is composed of two protein complexes: mTORC1 and mTORC2. Both are involved in anabolic metabolism, especially protein biosynthesis. As with insulin-growth factor 1, a reduction of mTOR activity extends lifespan in model organisms such as yeast, worms, mice, and flies. mTORC1 inhibition extends longevity by inducing mitophagy (degradation of mitochondria by autography) hence increasing mitochondria populations and slowing down cellular senescence. Studies on lung epithelial cells have shown that the mTOR1/ peroxisome proliferator-activated receptor gamma coactivator 1-alpha and transcription factor YY-1 pathway triggers mitochondrial biogenesis and hence increases mitochondrial function. The resulting excess generation of reactive oxygen species induces cellular senescence of the lung epithelial cells; consequently, senescent lung epithelial cells trigger the pathogenesis of pulmonary fibrosis. Scientists have shown the introduction of the pharmacologically active agent rapamycin, which inhibits the mTOR1 pathway, not only reduces cellular senescence in the lung epithelial cells but also reimposes mitochondrial homeostasis when that homeostasis has declined with age. However suppression of mTOR expression is not always helpful; in vivo studies in mice have shown that mTOR inhibition can cause health complications such as insulin insensitivity and cataracts.
Sirtuins are a class of proteins; they catalyze the removal of acetyl groups from other proteins and take part in catabolic metabolism. In vivo studies in mice have shown that the upregulation of SIRT6 genes increases longevity by facilitating an efficient DNA repair network, thus suppressing the start of cellular senescence. Studies in mice have also shown that the overexpression of SIRT3 genes promotes cell regeneration, especially among hematopoietic cells, thereby inhibiting cellular senescence and premature aging. SIRT1 is a class of proteins that mainly affect healthspan rather than lifespan by obstructing the pathogenesis of some age-related pathologies. Studies in model organisms have shown that the overexpression of SIRT1 genes may slightly extend longevity. SIRT2 is another kind of Sirtuin protein that extends lifespan in model organisms such as worms and mice. Calorie restriction and physical exercise elevate NAD+ levels thereby increasing Sirtuins activity. Supplementation and use of pharmacological agents that inhibit enzymes that deplete NAD+ ends up increasing the concentration of NAD+.
AMPK is an enzyme that regulates energy consumption at the cellular level. AMPK (AMP-activated protein kinase) is activated by an increase of ADP (adenosine diphosphate) concentration as a result of a subsequent drop in ATP (adenosine triphosphate) levels. A rise in AMP (adenosine monophosphate) concentration also activates AMPK. Upon activation, AMP-activated protein kinase replenishes ATP supplies by triggering fatty acid and glucose uptake as well as suppressing biosynthetic processes that exhaust ATP (this includes protein synthesis, gluconeogenesis, and lipid biosynthesis). AMPK levels are therefore elevated when nutrients are deficient. Studies have shown that an increase of AMPK activity promotes longevity just as sirtuins do.
In vivo studies in mice administered metformin indicated that this diabetes drug enhances longevity by increasing AMPK activity. Other studies show that calorie restriction - reduced diet - increases the activity of AMPK and extends lifespan in animals. AMP-activated protein kinase inhibits NF-?B signaling and inflammation. The decline of AMPK activity consequently increases the rate of inflammation and the levels of cellular and oxidative stress. It also impairs autophagy clearance. Cellular and oxidative stress might lead to cellular senescence while the imbalance between mitochondrial biogenesis and autophagy may result in mitochondrial dysfunction consequently leading to the pathogenesis of age-related maladies.
The balance between mitochondrial biogenesis and mitophagy (destruction of mitochondria by autophagy) establishes mitochondrial homeostasis. When the rate of mitochondrial degradation is higher than the rate of proliferation the resulting mitochondrial deficit leads to the rise of age-related pathologies, cellular senescence, and untimely aging.
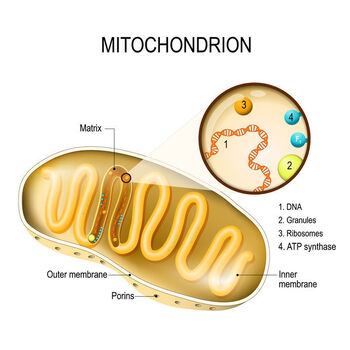 DNA in the mitochondria mutates ten times faster than nuclear DNA does, and the repair machinery for mitochondrial DNA is less efficient than the nuclear DNA repair network. The spontaneous generation of free radical species in the mitochondria makes the organelle prone to degradation - this increases the risk of mitochondrial genome instability. Reactive oxygen species may induce mutations in the mitochondrial DNA, leading to the aberrant transcription of genes. Defective protein synthesis facilitates the activation of mitophagy mediating pathways hence creating an imbalance between the rates of degradation and proliferation in the mitochondria.
DNA in the mitochondria mutates ten times faster than nuclear DNA does, and the repair machinery for mitochondrial DNA is less efficient than the nuclear DNA repair network. The spontaneous generation of free radical species in the mitochondria makes the organelle prone to degradation - this increases the risk of mitochondrial genome instability. Reactive oxygen species may induce mutations in the mitochondrial DNA, leading to the aberrant transcription of genes. Defective protein synthesis facilitates the activation of mitophagy mediating pathways hence creating an imbalance between the rates of degradation and proliferation in the mitochondria.
Mitochondria regulate essential cellular processes such as oxidative balance, iron and calcium homeostasis, apoptosis, cell regeneration, energy production, and the balance between oxidative species (e.g. free radicals) and the cell’s ability to handle those species (by introducing anti-oxidants). Mitochondria also play role in innate immunity. Mitochondrial impairment therefore causes health complications and cellular senescence. Dysregulation of oxidative balance leads to oxidative stress which triggers the genesis of senescence-associated secretory phenotype
Mitochondrial dysfunction is linked to cardiovascular pathologies such as hypertension, heart failure, ischemia-reperfusion injury, and atherosclerosis. The depletion of energy supply and impaired reactive oxygen species production as a result of mitochondrial dysfunction leads to the development of cardiovascular disorders.
Mitochondrial impairment permits uncontrolled reactive oxygen species generation which can lead to metabolic disorders such as diabetes. DNA damage aggregation as a consequence of excess oxidative stress triggers cellular senescence, and agglomeration of senescent cells inhibits homeostasis and tissue regeneration thereby giving rise to metabolic dysfunction pathologies such as diabetes.
Mitochondrial homeostasis is essential in the coordination of immune responses, especially for innate immune system signaling. When a body loses mitochondrial homeostasis it is more susceptible to viral and bacterial infections. Chronic viral infections like HBV (Hepatitis B) and HCV (Hepatitis C) infections persist in people suffering from mitochondrial dysfunction.
When the mitochondrial system does not function correctly, large quantities of reactive oxygen species can form, causing an imbalance between the level of antioxidants and reactive oxygen species. An excess of free radicals causes oxidative stress - this stress induces chronic cellular senescence and triggers the pathogenesis of maladies such as musculoskeletal diseases, neurobehavioral disease, and psychiatric disorders.
There’s no known cure for mitochondrial dysfunction; however, symptoms can be managed and treated by exercise, a vegetable-rich diet. and antioxidant vitamins such as thiamine B1 and riboflavin B2. Dysregulation of nutrient-sensing pathways can be treated by pharmacological agents such as rapamycin and mTOR inhibitors.
References